News







Exercise At Home: Tips And Care For Your Training At Home
July 21, 2021Want to train in the comfort of your home? Great, but you need to be careful not to get hurt...
Facts You Should Know About Knee Pain
May 20, 2021What you should Eat and Avoid for your Psoriasis?
January 28, 2021What’s Mix Fit Training?
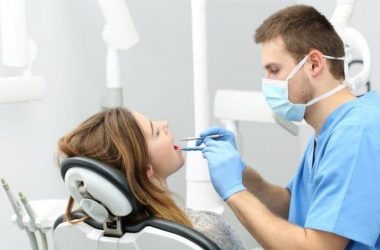
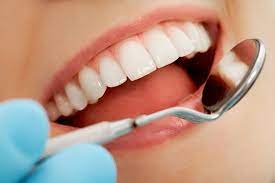
February 12, 2020How is a dental crown done? Temporary Crown vs. Permanent Crown
July 25, 2022Sometimes, one’s teeth get damaged, or a crack happens, decayed...
What Ethical Issues Arise When Dentists Provide Care For Older People?
October 25, 2021The older generation has the worst oral health in society,...
Teens and Teeth: Most Common Oral Health Obstacles to Tackle
February 10, 2021Exercise At Home: Tips And Care For Your Training At Home
July 21, 2021Want to train in the comfort of your home? Great, but you need to be careful not to get hurt...
Negative Effects Of Reduced Carb Diets
February 12, 2020Grapefruit Diet
February 12, 2020Top Internet Dieting Sources
February 12, 2020Slim Down – Rapidly and become Healthy With This Particular Diet
February 12, 2020Top Virtual TRT Solutions: Exploring the Best Online Options
April 13, 2024Pathways to Prosperity: Holistic Approaches to Overcoming Addiction
February 12, 2024The Pros and Cons of Anavar: A Must-Read Before Purchase
January 9, 2024Understanding Suboxone Treatment and its Benefits
May 20, 2023Tips On How To Use Gelatin
November 25, 2021Diet gelatin must be prepared with hot water as instructed on the package and can be consumed between the day's main meals or as an...
Halal gelatin
August 24, 2021The processing of gelatin generally involves the extraction of collagen from animal’s skin and bones. Standard gelatin is not permissible if you obey Islamic laws....
Delicious Camping Breakfast Recipes For Your Next Outdoor Trip
May 24, 2021If you’re going camping, you need to think of great ways to start your day right. One of the ideal ways is by having a...